Archive
Accenture Doctor’s Survey: The Digital Doctor is “In”
Accenture Eight-Country Survey of Doctors Shows Significant Increase in Healthcare IT Usage: The 2012 survey among 3,700 doctors in eight countries reveals that today’s doctors are going digital—now more than ever before. In fact, the survey shows a spike in healthcare IT usage across all countries surveyed (Australia, Canada, England, France, Germany, Singapore, Spain and the United States).
See on www.accenture.com
Hospitals Offer Better Food As Patient Satisfaction Becomes More Important Under Federal Health Law – Kaiser Health News
Administrators say the focus on food has taken on extra importance since Medicare last year began paying them based partly on their patient satisfaction scores, a change that is part of the federal health care law known as Obamacare.
“Food service helps the overall experience,” said Jim McGrody, director of food and nutrition at Rex, as he inspected his kitchen cold room used for brining pickles, curing turkey pastrami and fermenting cabbage into sauerkraut. Several letters of praise from former patients hang in the kitchen.
— Good healthcare, not good food, should be the focus, but sloppy unappetizing food preparation doesn’t say much about the quality of the facility’s healthcare.
See on www.kaiserhealthnews.org
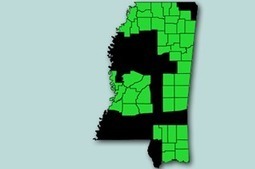
Thousands Of Mississippi Consumers May Not Be Offered Insurance Subsidies – Kaiser Health News
Tens of thousands of uninsured residents in the poorest and most rural parts of Mississippi may be unable to get subsidies to buy health coverage when a new online marketplace opens this fall because private insurers are avoiding a wide swath of the state. No insurer is offering to sell plans through the federal health law’s marketplaces in 36 of the state’s 82 counties, including some of the poorest parts of the Delta region, said Mississippi Insurance Commissioner Mike Chaney. As a result, 54,000 people who may qualify for subsidized coverage would be unable to get it, estimates the Center for Mississippi Health Policy, a nonpartisan research group.
See on www.kaiserhealthnews.org
Private commercial insurance companies are making this decision to deny healthcare coverage to thousands of poor rural Mississippians. This is not the fault of Obamacare. What is the solution – to give those people access to healthcare or not. State legislatures can no longer ignore the poor — the point is why should the private healthcare insureres be allowed to pick and choose like this – if they want to be licensed in Mississippi, they should be required to provide coverage throughout the state.
The Cost Disease : Why Computers Get Cheaper and Health Care Doesn’t
The idea behind Mr Baumol’s theory revolves around the fact that “productivity is increasing in all sectors of the economy, so it takes less time, man power and money to create things.” However in industries like computing, manufacturing and biotech, productivity has increased at a much faster rate compared with service industries such as healthcare, catering & education. In these industries the product on offer or service being provided is customised, therefore has an irreducible labour component as a result.
Cars can be made by robots in a high tech factory because each model is almost completely standardised by the manufacturer. However, robots cannot perform neurosurgery, heart transplants or kidney replacements which are non standardised and require different processes and components every time.
See on www.zesty.co.uk
The Gulf Between Doctors and Nurse Practitioners
Nurse practitioners believe that they can lead primary care practices and admit patients to a hospital and that they deserve to earn the same amount as doctors for the same work. Physicians disagree.
For several years now, health care experts have been issuing warnings about an impending severe shortfall of primary care physicians. Policy makers have suggested that nurse practitioners, nurses who have completed graduate-level studies and up to 700 additional hours of supervised clinical work, could fill the gap.
Already, many of these advanced-practice nurses work as their patients’ principal provider. They make diagnoses, prescribe medications and order and perform diagnostic tests. And since they are reimbursed less than physicians, policy makers are quick to point out, increasing the number of nurse practitioners could lower health care costs.
See on well.blogs.nytimes.com
Online health communities improve chronic care quality
Online health communities can be powerful tools for addressing chronic care issues as the number of people afflicted with such ailments rises, according to a study published this week in the Journal of Medical Internet Research.
For the study, researchers define online health communities (OHCs) as Internet-based platforms that unite a group of patients, a group of professionals, or both, using blogs, chats, forums and wikis. In this case, the researchers–from Radboud University Medical Centre in the Netherlands–illustrated using OHCs for ParkinsonNet, a professional network made for participants with Parkinson’s disease in which providers deliver patient-centered care.
ParkinsonNet utilized community managers; in this case, it was a marketing and communications expert. The community manager distributed posters, information pamphlets, and “business cards” to patients and health professionals as part of educating people about the OHC.
See on www.fiercehealthit.com
New direction for Medicaid in Alabama
About 120,000 Medicaid patients in the Shoals and Tennessee Valley will receive most of their health care from a network of willing providers within a 10-county region beginning in late 2016
The new direction for the state agency is part of a plan legislators approved earlier this year to control Medicaid’s ballooning costs.
State leaders plan to turn Medicaid from its current fee-for-service model to a managed care approach, beginning in fiscal 2017.
To make the transition, Medicaid officials are splitting the state into five areas where Regional Care Organizations — largely run by healthcare providers — will operate.
“The (Regional Care Organizations) came about because we’ve been on a fee-for-service type system with Medicaid, which doesn’t encourage providers to maximize efficiencies,” said Rep. Ed Henry, R-Hartselle, one of several lawmakers on Gov. Robert Bentley’s Medicaid study commission.
“This reform measure is to try to put efficiencies in Medicaid,” he said. “We pay providers a set amount per patient and if they deliver that care for cheaper, they make money. If they don’t, they lose money.”
David Spillers, CEO of Huntsville Hospital, said the regional organizations, or RCOs, will be a complete change in how Medicaid providers are reimbursed. The Huntsville Hospital system includes 12 medical facilities in north Alabama, including Helen Keller Hospital in Sheffield.
See on www.timesdaily.com
Physician EHRs: Make patient data work for you – amednews.com
Managing the data deluge an electronic health system provides can be a seemingly onerous task, but corralling the information will improve your practice.
Thanks to electronic health records and requirements that doctors use those systems to collect and share data, physician practices have easy access to information they never had before. The data, experts say, hold a lot of power. They can transform the way physicians treat patients and run their practices.
Since the rise of EHRs, much of the talk about patient data has been geared toward so-called big data used by insurance companies, researchers and large health systems to conduct large-scale research projects, guide best practices and determine population-based health statistics. But the data that go into those repositories originate inside physician practices. Experts say that in addition to sending the data along for outside projects, the information collected within a practice’s four walls can be used for its own data projects.
Practices already are collecting and reporting certain data measurements to meet requirements of the meaningful use incentive program. But many have not used the data beyond submitting the required reports, because they probably don’t know where to start.
See on amednews.com
Independence comes at price many doctors still willing to pay – amednews.com
Physicians in private practice say they are struggling financially compared with employed peers, but that the sacrifice is worth the autonomy.
See on amednews.com
Serious Medicine Strategy: House Majority Leader Eric Cantor Shifts the Paradigm on Healthcare–From Cuts to Cures.
House Majority Leader Eric Cantor (R-VA) said on Wednesday: “If you cure disease, you no longer have to spend dollars towards treating the symptoms … of those diseases.”
Bingo. Of course, cures are cheaper than care. It’s cheaper to beat than to treat. That was the lesson of polio. A cure is cheaper than care.
If we want to “bend the curve” on healthcare costs–and we all do–this is the right way to do. Also the only humane way.